Epidermal growth factor receptor (EGFR) gene mutation is the most common driver gene mutation in non-small cell lung cancer. At present, there are three generations of EGFR targeted drugs, including the first generation of erlotinib and gefitinib, the second generation of afatinib and dactinib, and the third generation of ositinib and vometinib. EGFR targeted drug therapy is the standard of first-line treatment for advanced non-small cell lung cancer with EGFR gene mutation. However, almost all patients will eventually develop disease progression due to acquired resistance to targeted drugs.
Why are EGFR targeted drugs resistant? What are the mechanisms of drug resistance? What treatment measures can be used after drug resistance? Today, the editor will give you an introduction to the inventory.
What are the mechanisms of EGFR targeting drug resistance?
EGFR can transmit extracellular signals to cells, and the downstream signaling pathway is complex (Fig. 1). The overexpression of this pathway caused by EGFR gene mutation is an important driver of abnormal cell proliferation and carcinogenesis.
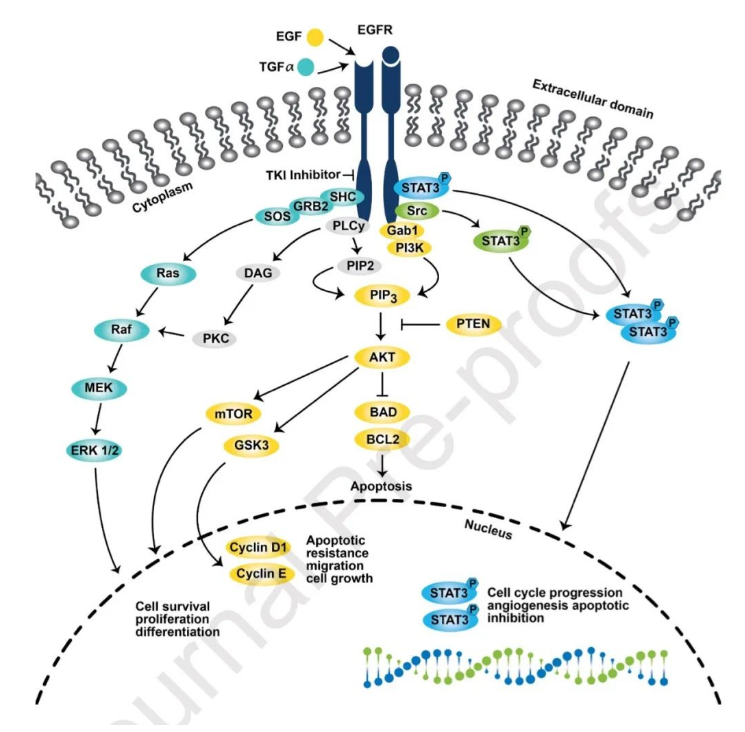
Figure 1. EGFR signaling pathway [1]
There are two mechanisms of EGFR targeting drug resistance. The first one is dependent on EGFR and involves secondary mutation of EGFR; The second is EGFR independent, including mutations and histological transformation that bypass EGFR signaling.
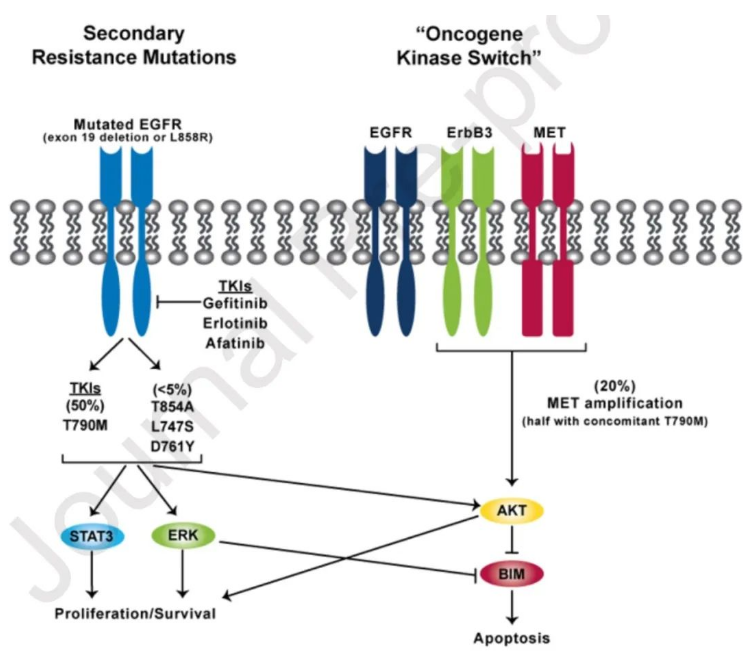
Figure 2. two types of resistance mechanisms of EGFR targeted drugs: secondary mutation and signaling bypassing EGFR
EGFR secondary mutation. Usually, a targeted drug can only target specific types of gene mutations, such as the first and second generation EGFR targeted drugs targeting exon 19 deletion mutation or L858R mutation, and the third generation ositinib targeting T790M mutation. One of the important mechanisms of EGFR targeted drug resistance is that additional mutations appear in this gene, bypassing the inhibitory effect of targeted drugs. For example, the most common resistance mechanism of the first and second generation targeted drugs is the T790M mutation. For example, 10% - 26% of the patients receiving second-line ositinib have grade III c797s resistance mutations. Among the patients receiving first-line ositinib treatment, about 7% of the patients had tertiary resistance mutations;
Bypassing the signaling of EGFR. EGFR independent mechanisms of drug resistance include amplification of met, HER2 and other genes; Fusion of ret; Mutations in KRAS, MEK or PI3K; And transformation to small cell lung cancer. MET oncogene amplification accounts for 5% - 20% of the acquired resistance of EGFR targeted drugs, and this form of resistance can be produced by first-line and second-line ositinib treatment. In addition to met, another frequently amplified gene is HER2, which encodes erbB2 receptor tyrosine kinase. HER2 amplification can activate MAPK and PI3K pathways. Compared with the third generation targeted drugs, HER2 amplification is more common in the first generation targeted drug resistance. Although the frequency of transformation to small cell lung cancer is not high, it is a relatively difficult type, with few treatment methods and relatively poor prognosis.
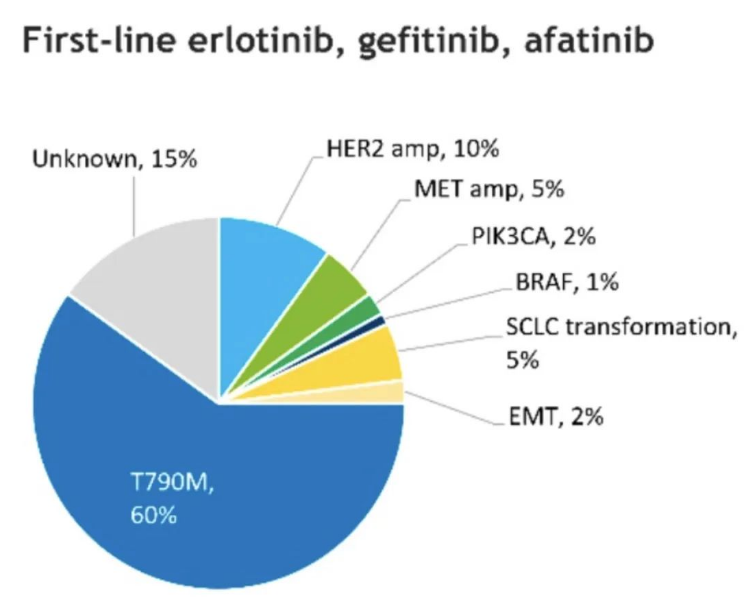
Figure 3. common resistance mutations after first-line erlotinib, gefitinib, and afatinib treatment
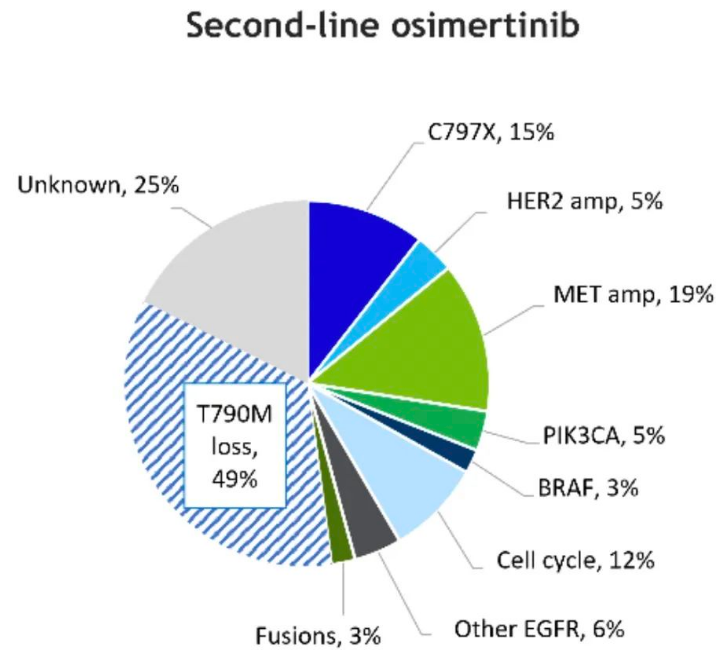
Figure 4. common drug resistance mutations after second-line ositinib treatment

Figure 5. common resistance mutations after first-line ositinib treatment
Therapeutic options after targeted drug resistance
Targeted drug sequential therapy. Sequential treatment with different EGFR targeted drugs has good or bad results. For example, in one study, erlotinib was used to treat patients with resistance to gefitinib, with an overall survival of 5-11 months and limited benefits. In another study, after treatment with erlotinib or gefitinib, a T790M drug-resistant mutation was generated, and the patient received ositinib treatment. The median overall survival was 26.8 months, and the benefit was not bad;
Combination therapy. After targeted drug resistance, the common coping measures at present are combined with other therapies, including chemotherapy, immunotherapy, anti angiogenic targeted drugs, etc. At present, combination chemotherapy is the standard treatment, but patients do not always benefit from it. The clinical trial results of combined immunotherapy are not optimistic, which may be due to the low expression of PD-L1 in tumors or the strong immunosuppressive microenvironment in tumors with EGFR mutations. Anti angiogenic targeted drugs targeting vascular endothelial growth factor receptor (VEGFR) signaling have good effects in treating other cancers, and have shown certain potential in non-small cell lung cancer. Many clinical trials are being carried out.
New drug development
In view of the different mechanisms of the two EGFR targeted drug resistance, the current drug development also focuses on these two aspects.
The fourth generation of EGFR targeted drugs. C797s mutation is the most common mechanism of resistance to ositinib. At present, there are many fourth generation EGFR targeted drugs (eai045, blu-945, blu-701, bbt-176) under development. Preliminary clinical trial data show that the fourth generation therapy has a certain effect, and more clinical data are expected.
Targeted drugs for met. Met is an important target of EGFR targeted drug resistance. At present, there are many approved drugs, including capmatinib, tepotinib, cabozantinib and amivantamab.
Targeted drugs against HER2. HER2 amplification was observed in approximately 10% of tumors that progressed after first-line erlotinib or gefitinib treatment; Less after resistance to ositinib. Preclinical studies have shown that antibody drug conjugate (ADC) trastuzumab emtansine (t-dm1) can overcome resistance to ositinib. Another antibody drug conjugate, trastuzumab deruxtecan (t-dxd), showed good antitumor activity in patients with HER2 expression or HER2 mutation.
Summary
Although the frequently used strategy to combat EGFR targeted drug resistance is still the standard platinum chemotherapy, many other combination therapies have also shown some benefits. In addition, clinical trials of promising new drugs targeting common drug resistance mechanisms such as met and HER2 have also attracted more and more attention. For patients with EGFR targeted drug resistance, gene sequencing at the time of initial progression is helpful to determine the relevant drug resistance mechanism and symptomatic drug use.
Source link:
https://www.cn-healthcare.com/articlewm/20220824/content-1423924.html